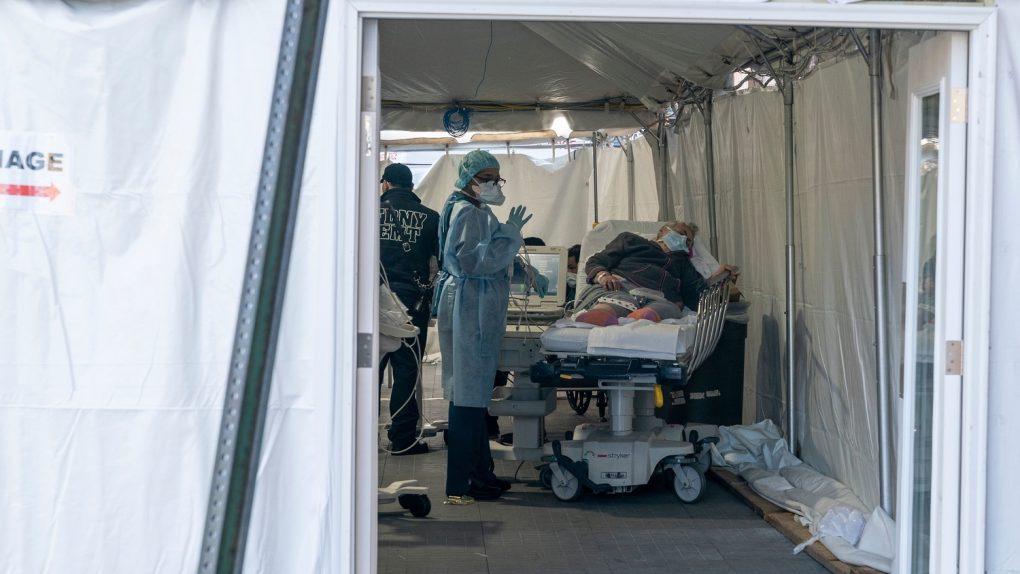
- Researchers have examined the detailed medical records of 85 patients who died in Wuhan of COVID-19, looking for commonalities.
- They searched for comorbidities, symptoms, and test results that could indicate a poor coronavirus prognosis.
- The findings could be used to adapt protocols and therapies for COVID-19 patients that may be most at risk of developing a severe coronavirus case.
- Visit BGR’s homepage for more stories.
Scientists may be scrambling for COVID-19 cures and vaccines right now, but the harsh reality is that the novel coronavirus will continue to claim lives for many weeks and months to come. Some countries managed to flatten the curve and keep the death toll in check through a combination of social distancing measures and aggressive testing. In contrast, others have been overwhelmed by the increasing number of COVID-19 patients in the past few weeks. Nearly 76,000 have people died around the world as of Tuesday morning stats, out of more than 1,335,000 confirmed patients.
Some medical professionals are trying to improve protocols for people who experience life-threatening COVID-19 infections by looking at what happened in fatal coronavirus cases. A study that used artificial intelligence recently discovered three signs that increase the likelihood of a COVID-19 patient developing respiratory complications that would require ventilation. Now, a new study from China and the US analyzed a group of fatal COVID-19 patients, looking for commonalities between those cases.
The brand new study was published online in the American Thoracic Society’s American Journal of Respiratory and Critical Care Medicine (via Medical Xpress): Clinical Features of 85 Fatal Cases of COVID-19 From Wuhan: A Retrospective Observational Study.
Researchers from the US and China looked at the electronic health records of 85 patients who died in two hospitals in Wuhan. That’s the region where the novel coronavirus pandemic started a few months ago. They looked at their medical histories, exposure to coronavirus, and other chronic diseases. They also analyzed COVID-19 symptoms, laboratory results, CT readings, and the clinical evolution of these patients.
They made several discoveries that could help physicians adapt treatment and prioritize resources going forward.
The researchers concluded that the highest number of deaths occurred in males over 50 with other chronic diseases. Hypertension, diabetes, and coronary heart disease were the most common comorbidities. The most common in COVID-19 cases that were ultimately fatal included fever, shortness of breath, and fatigue. Complications included respiratory failure, shock, acute respiratory distress syndrome (ARDS), and cardiac arrhythmia.
Blood test abnormalities included eosinophilopenia, which seemed to indicate a poor prognostic. Eosinophil counts are reduced in severe respiratory infections. The early onset of shortness of breath was also a common symptom for these cases. Wuhan doctors treated most of these patients with several combinations of drugs, including antibiotics, antivirals, and glucocorticoids. Some of them were given intravenous immunoglobulin or interferon alpha-2b.
The medical records of the 85 patients revealed that the respiratory symptoms may not develop until a week after infection. But once they do, the deterioration is rapid:
The effectiveness of medications such as antivirals or immunosuppressive agents against COVID-19 is not completely known. Perhaps our most significant observation is that while respiratory symptoms may not develop until a week after presentation, once they do there can be a rapid decline, as indicated by the short duration between time of admission and death (6.35 days on average) in our study.
The researchers also noted that the characteristics they identified might not be valid for all regions. Factors like genetics and the mutation of the virus could alter the course of fatal cases in other areas.