- Can coronavirus symptoms predict whether a patient will develop a severe case of COVID-19? A new study says that’s precisely the case, providing six different clusters of symptoms that COVID-19 patients can experience.
- Using data from an app that requires patients to log their symptoms, COVID-19 diagnosis status, and progress of the illness, scientists at King’s College London used machine learning to group symptoms together.
- Using patient characteristics like age, sex, and medical conditions combined with symptom data from the first five days after onset, the scientists think they can predict nearly 80% of the time a patient would require respiratory support.
One of the most annoying things about the novel coronavirus is the lack of a telling symptom or group of symptoms that could help us when diagnosing the illness. The sudden loss of smell and taste is an odd exception, but not all the people get it, so it’s not enough. Not to mention that many people who do get infected will not experience any symptoms at all. That’s why testing is so necessary. It’s the only way to confirm infection.
But some scientists used a mobile app and machine learning to track symptoms and divide them into several groups. The aim of the work was to see whether they could use groups of symptoms to predict severe COVID-19 cases that can develop complications. If the study can be verified by additional research, it could give physicians ample time to prevent the onset of complications. Moreover, patients would know when to hurry to the hospital to seek proper COVID-19 treatment rather than attempting to ride out the disease at home.
“Anything you can do earlier to stop people coming in half-dead is going to increase the chance of survival and also stop clogging up hospital beds unnecessarily,” Professor Tim Spector of King’s College London told The Guardian. The study has been published in medRxiv, which means it hasn’t been peer-reviewed.
The researchers looked at data from a mobile app that has more than four million users and included 1,653 users in the study who tested positive for COVID-19 and then reported symptoms and provided updates on their health status. Of those, 383 made at least one trip to the hospital, and 107 needed oxygen or ventilation.
The researchers applied machine learning algorithms to the data to explore whether the 14 symptoms they monitored can cluster together, and they identified six different groups of COVID-19 patients. Each cluster was associated with a particular outcome, and that’s why the scientists think they know which combination of symptoms can be indicative of serious illness.
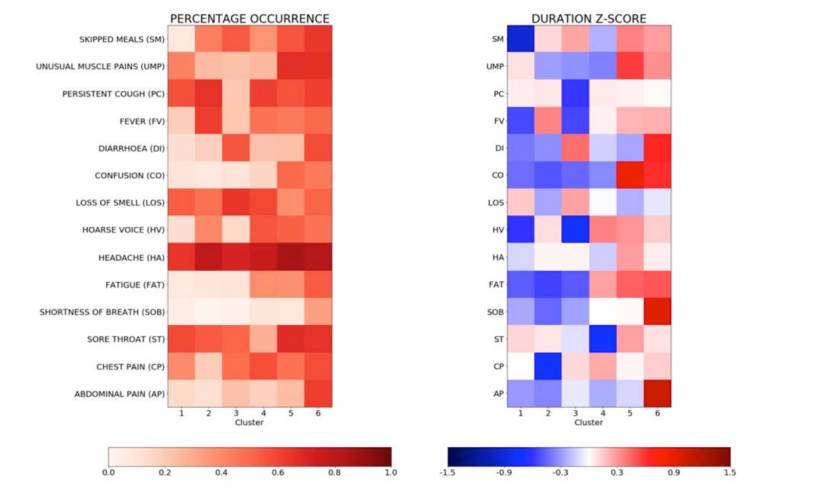
These are the six coronavirus symptoms groups that the King’s College London team identified:
- Cluster 1 (462 patients): Upper respiratory tract symptoms like a persistent cough, and muscle pain. Some 1.5% of patients needed respiratory support, and 16% of them made at least a trip to the hospital.
- Cluster 2 (315 patients): Upper respiratory tract symptoms, a higher frequency of skipped meals, and fever. Of this group, 4.4% of patients needed respiratory support, and 17.5% made one or more visits to the hospital.
- Cluster 3 (216 patients): Gastrointestinal symptoms like diarrhea, but few other symptoms. 3.7% of patients in this group needed respiratory support, and 24% made at least one visit to the hospital.
- Cluster 4 (280 patients): Early signs of severe fatigue, continuous chest pain, and cough. 8.6% of patients needed respiratory support, and 23.6% went to the hospital at least once.
- Cluster 5 (213 patients): Confusion, skipped meals, severe fatigue. 9.9% of patients needed respiratory therapy, and 24.6% went to the hospital at least once.
- Cluster 6 (167 patients): Marked respiratory distress, the onset of breathlessness, chest pain, confusion, fatigue, gastrointestinal symptoms. As many as 20% of the patients in this group needed respiratory support, and 45.5% went at least once to the hospital.
The first two clusters of symptoms represent milder forms of COVID-19, according to the team. The researchers repeated the work with data from 1,047 other app users, adding headaches and the loss of smell and taste. The latter appeared in all clusters but was longer-lasting in milder cases.
Using the data from the first five days of reported symptoms, and information such as patient age, sex, and other medical conditions, the team said it could predict whether a patient would need respiratory support 79% of the time. Patient characteristics alone would result in a success rate of less than 70%.
Like any other COVID-19 study, this promising work could benefit from more research. If the data is accurate, then physicians might be able to predict which patients are likely to develop COVID-19 complications and save even more lives. It all hinges on the patient’s ability to track the symptoms correctly and relay them to caregivers. The team concluded that the average time to get to the hospital is 13 days. The only objective way to do this is with the help of a smart device and logging the data promptly. An app would help even more.
“By recording all the symptoms and when they occur in something like a medical app, you can significantly increase the ability to predict who is going to need hospital support, and potentially save lives,” Spector said. But people would have to remember to log symptoms and stick with it no matter how sick they get.








